Overview
After your Achilles tendon decides to play snap instead of support, recovery unfolds across distinct phases spanning 6-12 months: from initial immobilization (0-6 weeks), to progressive weight-bearing (6-12 weeks), functional restoration (3-6 months), and finally returning to full activities (6-12+ months). The timeline varies based on injury severity, treatment approach (surgical vs. non-surgical), age, rehabilitation adherence, and lifestyle factors, with most patients achieving 80-90% return to pre-injury activity levels despite some residual differences in calf strength.
Table of Contents
- Understanding Achilles Tendon Injuries
- Immediate Post-Injury Phase (0-2 Weeks)
- Early Recovery Phase (2-6 Weeks)
- Mid Recovery Phase (6-12 Weeks)
- Advanced Recovery Phase (3-6 Months)
- Return to Sports and Full Activity (6-12+ Months)
- Factors That Affect Healing Time
- Long-term Outlook
- Conclusion
- Frequently Asked Questions
The Achilles tendon, the strongest tendon in your body, plays a crucial role in your daily mobility. When this mighty cord connecting your calf muscles to your heel bone tears, your life temporarily grinds to a halt. The burning question becomes: how long does a torn Achilles take to heal?
Recovery from an Achilles tear is highly individual. Some people bounce back in months, while others need a year or more to fully heal. This timeline depends on several factors, including injury severity, treatment approach, age, overall health, and rehabilitation adherence.
As an orthopedic specialist with over 15 years of experience treating Achilles injuries, I’ve guided hundreds of patients through this challenging journey. Let me walk you through what to expect during each phase of healing and provide realistic timeframes for recovery milestones.
Understanding Achilles Tendon Injuries
Before discussing healing timelines, it’s essential to understand what you’re dealing with. Achilles tendon injuries exist on a spectrum, from minor strains to complete ruptures, each with distinct recovery trajectories.
A partial tear involves damage to some tendon fibers while others remain intact. These injuries typically result from overuse, with microscopic tears accumulating over time. Think of it as gradually fraying a rope rather than snapping it completely.
Complete ruptures occur when the tendon tears entirely, creating a gap between the separated ends. These typically happen suddenly—often with an audible “pop”—during activities requiring explosive movements. You’ll immediately lose the ability to push off with your affected foot.
The most common causes include:
- Sports involving sudden acceleration or direction changes (basketball, tennis, soccer)
- Abrupt increases in training intensity
- Poor flexibility or previous tendinopathy
- Certain medications (particularly fluoroquinolone antibiotics)
- Age-related tendon degeneration
According to a comprehensive study in the Journal of Foot and Ankle Research, the severity of your injury significantly impacts healing time. A mild strain might have you back on your feet in weeks, while complete ruptures typically require months of rehabilitation.
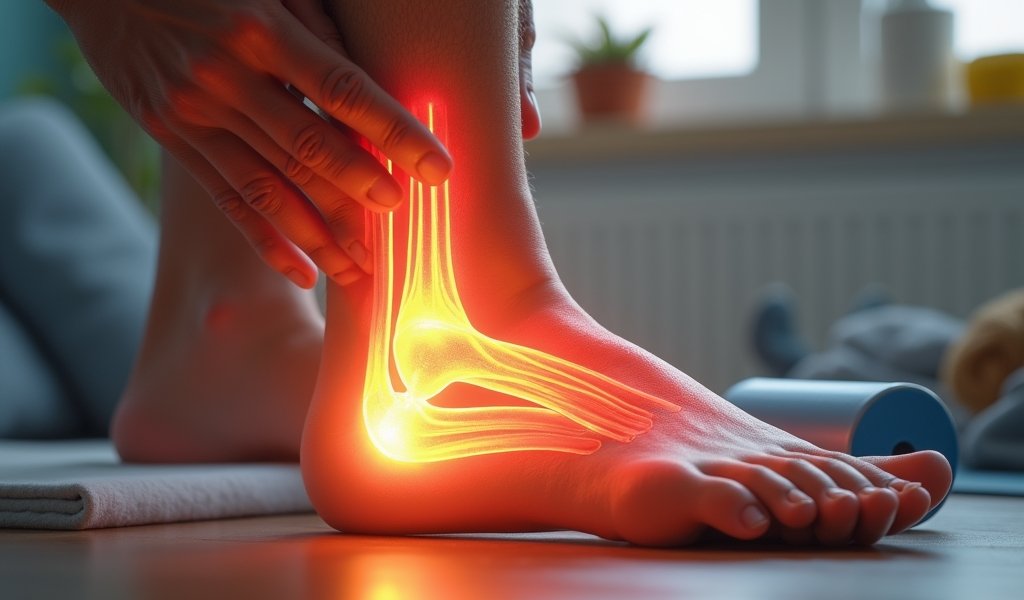
Immediate Post-Injury Phase (0-2 Weeks)
The moment that telltale “pop” occurs, your healing clock starts ticking. The first two weeks are critical for proper diagnosis and treatment planning.
Immediately after injury, follow the R.I.C.E. protocol: Rest, Ice, Compression, and Elevation. This approach helps manage pain and swelling while preventing further damage. Ice the injured area for 20 minutes several times daily, use compression bandages between icing sessions, and keep your foot elevated above heart level whenever possible.
During this phase, your doctor will likely perform a physical examination, including the Thompson test (squeezing your calf to see if your foot moves), and order imaging studies like ultrasound or MRI to determine the extent of the tear.
One of the most significant decisions happens now: surgical or non-surgical treatment? This choice substantially affects your recovery timeline. The Mayo Clinic notes that while complete ruptures were traditionally repaired surgically, recent research shows that even complete tears can heal well without surgery in certain patients.
Your doctor will consider factors including your age, activity level, and general health when making recommendations. Surgical repair may offer a slightly lower risk of re-rupture but comes with surgical risks. Non-surgical treatment avoids those risks but may result in slightly reduced strength.
For pain management, your doctor may prescribe medications and provide crutches or a walking boot to keep weight off the injured tendon. This period can feel frustrating, but proper initial care sets the foundation for optimal recovery.
Early Recovery Phase (2-6 Weeks)
Welcome to the immobilization period—where patience becomes your superpower. During these weeks, your tendon begins its healing process by forming scar tissue to bridge the gap between the torn ends.
If you’ve had surgery, you’ll likely wear a cast or walking boot with your foot positioned to remove tension from the Achilles. For non-surgical treatment, you’ll typically be in a cast or boot with your foot initially pointed downward (equinus position), gradually moving to a neutral position as weeks progress.
Expect substantial limitations during this phase. Simple tasks like showering become complicated, and you’ll discover muscles you never knew existed as you adapt to crutches or knee scooters. As one of my patients humorously put it, “I never appreciated how challenging it is to carry coffee while on crutches—it’s practically an Olympic sport!”
Common challenges include:
- Muscle atrophy (significant calf shrinkage)
- Stiffness in the ankle and foot
- Persistent swelling and discomfort
- Psychological impact of limited mobility
Around weeks 4-6, depending on your treatment approach and progress, gentle rehabilitation typically begins. This might include range of motion exercises, light resistance training, and proprioception work. These early movements feel awkward at first but gradually become more natural as healing progresses.
Mid Recovery Phase (6-12 Weeks)
The mid-recovery phase marks an exciting transition as you begin bearing weight on your healing tendon. Progress becomes visibly apparent, boosting morale after weeks of limitation.
For most patients, weight-bearing activities begin gradually around 6-8 weeks post-injury. Initially, you’ll likely use a walking boot with a heel lift that decreases in height as your tendon adapts to increasing stretch. Your physical therapist becomes your most important ally during this phase.
A typical physical therapy protocol includes:
- Graduated weight-bearing exercises
- Resistance band work for strengthening
- Ankle mobility exercises
- Balance and proprioception training
Progress markers include decreased swelling, improving range of motion, and growing confidence when placing weight on your foot. However, this phase also brings potential setbacks. The temptation to do too much too soon is overwhelming when you start feeling better.
Remember, your tendon might feel ready for more activity before it’s structurally prepared—leading to the classic “two steps forward, one step back” recovery pattern. As I often remind my patients: “Your Achilles doesn’t care about your vacation plans or work deadlines—it heals according to biological timelines, not your calendar.”
Research in the Journal of Orthopaedic & Sports Physical Therapy shows that early controlled motion and progressive loading lead to optimal outcomes, but patience remains essential during this critical healing phase.
Advanced Recovery Phase (3-6 Months)
As you enter months 3-6, your recovery shifts focus from basic healing to functional restoration. The repaired tendon has formed a strong scar but now needs to regain elasticity, strength, and function.
This phase introduces more dynamic strengthening exercises including:
- Calf raises (progressing from two-legged to single-leg)
- Eccentric loading exercises (controlled lowering movements)
- Walking on various surfaces and inclines
- Low-impact cardiovascular activities like stationary biking and swimming
Around 3-4 months post-injury, most patients return to relatively normal walking mechanics, though often with residual morning stiffness. The joy of walking normally again after months of limping cannot be overstated—it’s like rediscovering a fundamental freedom.
Rebuilding calf muscle strength becomes a primary focus, as significant atrophy typically occurs during immobilization. Don’t be alarmed by the dramatic difference in size between your calves—this is expected and improves with consistent training.
By months 5-6, many everyday activities resume: climbing stairs normally, light hiking on even terrain, and moderate-intensity cycling. However, activities requiring explosive movements or significant impact remain off-limits for most patients at this stage.
Return to Sports and Full Activity (6-12+ Months)
The final phase of recovery spans from 6 months to potentially beyond a year, especially for competitive athletes or those with physically demanding occupations.
Return to sports follows a carefully graduated progression:
- Low-impact activities (swimming, cycling)
- Moderate-impact (elliptical training, fast walking)
- Higher-impact (jogging, tennis)
- Explosive movements (sprinting, basketball, volleyball)
Sport-specific rehabilitation becomes essential during this phase. A basketball player needs different preparation than a distance runner or dancer. Your physical therapist should tailor exercises to the specific demands of your preferred activities.
Preventing re-injury becomes paramount as you increase activity levels. Studies from Physio-pedia recommend these strategies:
- Proper warm-up routines
- Maintaining flexibility through regular stretching
- Continuing strengthening exercises even after returning to sport
- Using appropriate footwear and technique
- Avoiding sudden increases in training intensity
How do you know you’re ready for full activity? Look for these signs:
- Equal or nearly equal strength in both calves (measured by single-leg heel raises)
- Full, pain-free range of motion
- Ability to hop on the affected leg without pain
- Confidence in the leg during unpredictable movements
As one of my recovered athlete patients said, “My surgeon told me I’d be physically ready before I was mentally ready—and he was right. Trusting the healed tendon was harder than actually healing it.”
Factors That Affect Healing Time
If recovery timelines seem frustratingly variable, that’s because numerous factors influence your personal healing journey.
Age plays a significant role—younger patients typically heal faster due to better blood supply and cellular regeneration. However, this doesn’t mean older adults can’t achieve excellent outcomes; they may just need more time and patience.
Adherence to rehabilitation protocols dramatically impacts recovery speed. Patients who diligently perform their exercises and respect activity restrictions generally recover faster than those who push too hard or skip therapy sessions.
Nutrition deserves special attention during recovery. Your body needs adequate protein to build new tissue, vitamin C for collagen formation, zinc for wound healing, and sufficient calories to support the energy-intensive repair process. A well-balanced diet rich in whole foods provides the building blocks your healing tendon needs.
Lifestyle factors can either accelerate or impede recovery. Smoking significantly delays tendon healing by restricting blood flow and impairing tissue repair—potentially adding weeks or even months to recovery time. Adequate sleep, stress management, and maintaining a healthy weight all contribute to optimal healing conditions.
Long-term Outlook
After navigating the long road to recovery, what can you expect for the future?
Most patients achieve excellent functional outcomes following Achilles tendon ruptures, whether treated surgically or non-surgically. Approximately 80-90% of patients return to their pre-injury activity levels, though some notice subtle differences in their recovered leg.
Potential long-term considerations include:
- Slightly reduced calf strength (typically 10-20% less than the uninjured side)
- Mild tendon thickening at the injury site
- Occasionally, altered running mechanics
- Increased awareness of the need for proper warm-up and maintenance exercises
The re-rupture rate is relatively low at approximately 4-5%, with most re-injuries occurring either very early in the recovery process (due to non-compliance with restrictions) or during the return to sports phase (due to inadequate preparation).
For perspective, numerous professional athletes including Kobe Bryant and Demaryius Thomas have returned to elite competition following Achilles ruptures. While they often reported having to adapt certain aspects of their game, they successfully competed at the highest levels of their sports.
Conclusion
Healing a torn Achilles tendon follows a predictable sequence of phases, but with a timeline as individual as you are. For most people, the broad recovery arc spans 6-12 months, with functional walking resuming around 3-4 months and return to demanding activities occurring later.
Throughout this process, patience becomes your most valuable asset. The tendon heals according to biological timelines that cannot be rushed, regardless of your determination. Respecting the healing process ultimately leads to better long-term outcomes.
The most successful recoveries share a common approach: balancing determination with patience, working consistently on rehabilitation while respecting your body’s signals. Recovery isn’t linear—some days bring noticeable progress, while others seem frustratingly stagnant.
If you’re concerned about your recovery progression, don’t hesitate to consult with healthcare providers. Variations in individual healing are normal, but persistent pain, significant swelling, or inability to progress through expected recovery phases warrants medical attention.
Remember, healing an Achilles rupture isn’t just about physical recovery—it’s also a mental journey requiring adaptation and perseverance. With proper treatment and rehabilitation, you’ll find yourself back on your feet, perhaps moving differently but often with a newfound appreciation for the remarkable healing capacity of the human body.
Frequently Asked Questions
How long until I can walk normally after Achilles tear?
Most patients return to normal walking mechanics around 3-4 months post-injury. You’ll likely progress from non-weight-bearing to partial weight-bearing with a boot before transitioning to normal footwear.
Does surgical repair heal faster than non-surgical treatment?
Surgical and non-surgical approaches have similar overall healing timelines. The decision between treatments should be based on individual factors like age, activity level, and health status rather than speed of recovery.
When can I drive after an Achilles rupture?
If your left Achilles is injured (in cars with automatic transmission), you may be cleared to drive around 2-4 weeks. For right Achilles injuries, most patients return to driving between 6-12 weeks, once they can safely operate the pedals.
Will my calf ever look normal again?
Your calf will regain much of its size with consistent strengthening, but some permanent asymmetry is common. Most patients achieve 80-90% of their original calf circumference compared to the uninjured side.
Can I prevent another Achilles tear in the future?
Regular stretching, proper warm-up, appropriate footwear, and avoiding sudden increases in activity intensity can reduce re-injury risk. Maintaining calf strength through regular eccentric strengthening exercises provides additional protection.
