Overview
Hip replacement patients often experience buttock pain that could make sitting feel like you’ve accidentally backed into a porcupine at a nudist colony, but fear not—this discomfort is usually normal! The article explains that buttock pain after hip replacement commonly stems from muscle trauma, sciatic nerve irritation, or implant issues, and typically improves within 3-6 months through physical therapy, medication, and proper recovery management, though persistent or worsening symptoms warrant medical attention.
Table of Contents
- Understanding Buttock Pain After Hip Replacement
- Common Causes of Buttock Pain After Hip Replacement
- Normal Pain vs. Concerning Symptoms
- Diagnosing Post-Hip Replacement Buttock Pain
- Treatment Options for Buttock Pain
- Recovery and Pain Management Strategies
- Prevention Tips and Long-Term Care
- When to Seek Medical Help
- Conclusion
- Frequently Asked Questions
Understanding Buttock Pain After Hip Replacement
Hip replacement surgery offers life-changing relief for many patients suffering from severe hip pain and limited mobility. While this procedure has an impressive success rate, experiencing some discomfort during recovery is perfectly normal – including buttock pain, which affects approximately 15-30% of patients following surgery.
As an orthopedic specialist who’s guided hundreds of patients through hip replacement recovery, I can assure you that buttock pain doesn’t necessarily indicate something has gone wrong. Your body has undergone significant trauma and is adapting to a new artificial joint, which affects surrounding muscles, nerves, and tissues.
The causes of buttock pain after hip replacement range from typical healing responses to more serious complications requiring medical attention. Understanding these distinctions can help ease anxiety during recovery and ensure you seek appropriate care when needed.
Recovery from hip replacement is a journey unique to each patient, influenced by factors including surgical approach, pre-existing conditions, and individual healing capacity. Most patients find their physical wellness improves dramatically within 3-6 months, but complete tissue healing and adaptation to your new joint may take up to a year.
Common Causes of Buttock Pain After Hip Replacement
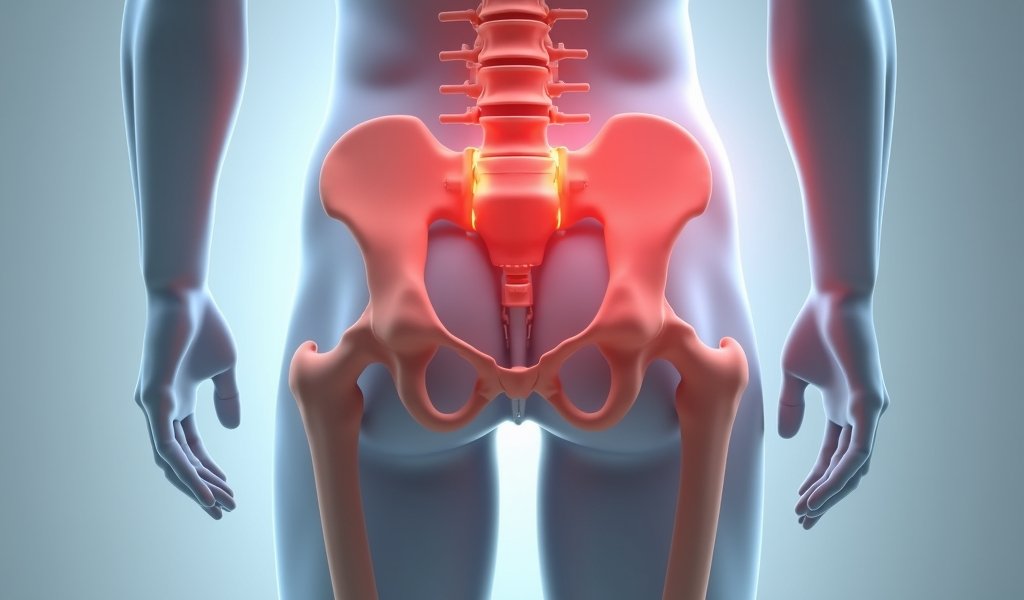
Understanding the specific cause of your buttock pain is crucial for effective treatment. Let’s explore the most common culprits:
1. Muscle Trauma and Inflammation
During hip replacement surgery, your surgeon must navigate through or temporarily detach muscles to access the hip joint. The gluteal muscles (forming your buttocks) are particularly affected in posterior approach surgeries. This necessary trauma creates inflammation and pain during healing.
Muscle pain typically feels like a deep ache or soreness that worsens with activity and improves with rest. This discomfort normally peaks 2-3 days after surgery and gradually improves over 6-12 weeks as tissues heal. Research published in the Journal of Orthopedic & Sports Physical Therapy shows that targeted physical therapy significantly accelerates muscle recovery.
2. Sciatic Nerve Irritation
The sciatic nerve runs from your lower back through your buttocks and down each leg. During surgery, this nerve may become irritated through stretching, compression, or inflammation of surrounding tissues. The posterior surgical approach presents a higher risk for sciatic nerve involvement.
Sciatic pain typically manifests as sharp, burning, or electrical sensations that may radiate down your leg. You might also experience numbness or tingling. Most nerve irritation resolves within 3-6 months as swelling subsides, though permanent nerve damage occurs in approximately 1% of cases.
3. Implant-Related Issues
Sometimes the artificial components themselves contribute to buttock pain. This may result from:
- Implant positioning that alters your biomechanics
- Prosthesis loosening (typically a later development)
- Leg length discrepancy creating muscle imbalance
- Metal sensitivity reactions (in 1-5% of patients)
Implant-related pain often feels deeper, may increase with specific movements, and typically doesn’t improve at the same rate as normal healing pain. Modern surgical techniques and planning have reduced these issues, but they remain important considerations.
4. Bursitis and Tendinitis
The trauma of surgery combined with altered movement patterns can irritate the bursae (fluid-filled cushioning sacs) around your hip joint. Trochanteric bursitis is particularly common after hip replacement and causes pain on the outer hip that may radiate to the buttock.
Similarly, tendons connecting muscles to bones can become inflamed (tendinitis) during recovery as you regain mobility. Both conditions typically respond well to targeted physical therapy, anti-inflammatory medications, and temporary activity modification.
5. Referred Pain
Sometimes buttock pain after hip replacement actually originates from a different source. Common referred pain sources include:
- Lower back problems (herniated discs, spinal stenosis)
- Sacroiliac joint dysfunction
- Pelvic floor disorders
Your surgeon and physical therapist will carefully evaluate these possibilities, especially if your buttock pain doesn’t follow the expected improvement pattern or has characteristics unusual for typical post-operative pain.
Normal Pain vs. Concerning Symptoms
Distinguishing between expected recovery discomfort and potential complications is crucial for proper healing. Here’s what you should know:
Normal Healing Pain
During normal recovery, your buttock pain should follow a predictable pattern:
- Most intense during the first 1-2 weeks
- Gradually improves week by week
- Typically worse with activity and better with rest
- Responds positively to prescribed pain management
- Allows for progressive improvement in function
This expected discomfort reflects your tissues healing and adapting to your new joint. Many patients describe it as similar to muscle soreness after intensive exercise. By 6-12 weeks post-surgery, this pain should be significantly reduced for most patients.
Concerning Symptoms
Watch for these warning signs that may indicate complications requiring medical attention:
- Severe pain that begins suddenly after a period of improvement
- Pain accompanied by fever, chills, or unusual drainage from the incision
- Significant swelling, redness, or warmth around the surgical site
- New onset of numbness, tingling, or weakness in the leg
- Pain that consistently wakes you from sleep
- Inability to bear weight on the affected leg
These symptoms could signal infection, dislocation, blood clots, or other serious complications that require prompt evaluation. According to the American Academy of Orthopaedic Surgeons, early intervention for complications significantly improves outcomes.
Every patient’s recovery timeline differs, but persistent or worsening pain beyond 3 months post-surgery warrants a follow-up with your surgical team. Trust your instincts – if something feels wrong, don’t hesitate to contact your healthcare provider.
Diagnosing Post-Hip Replacement Buttock Pain
When buttock pain persists beyond expected recovery timelines, your healthcare team will use several approaches to determine the cause:
Clinical Evaluation
Your surgeon or physical therapist will typically begin with a thorough physical examination, assessing:
- Pain patterns and triggers
- Range of motion in the hip joint
- Muscle strength and tenderness
- Gait analysis (how you walk)
- Neurological testing
The location, quality, and timing of your pain provide valuable diagnostic clues. For example, pain primarily with weight-bearing might suggest mechanical issues, while pain at rest could indicate inflammation or infection.
Imaging Studies
Various imaging techniques help visualize your hip replacement and surrounding structures:
- X-rays show implant positioning and potential loosening
- CT scans provide detailed 3D images of bone and implant relationships
- MRI (with special metal artifact reduction sequences) evaluates soft tissues
- Ultrasound assesses bursitis and tendon inflammation
- Bone scans detect areas of increased bone metabolism that might indicate infection or loosening
Your surgeon will select the most appropriate imaging based on your specific symptoms and suspected cause. Sometimes multiple imaging modalities are necessary for a complete picture.
Laboratory Tests
Blood tests help identify infection and inflammation:
- Complete blood count (CBC) screens for infection
- Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) measure inflammation
- In some cases, joint fluid analysis may be necessary
Elevated inflammatory markers don’t definitively diagnose specific conditions but help guide further investigation. These tests are particularly important when infection is suspected, as restoring health and wellness quickly is critical with prosthetic joint infections.
Diagnostic Injections
Sometimes targeted injections serve both diagnostic and therapeutic purposes. For example, if a lidocaine injection into the trochanteric bursa relieves your pain, this confirms bursitis as the cause. Similarly, spine injections might identify referred pain from back issues.
A comprehensive diagnostic approach ensures accurate identification of the underlying problem, allowing for targeted, effective treatment rather than simply managing symptoms.
Treatment Options for Buttock Pain
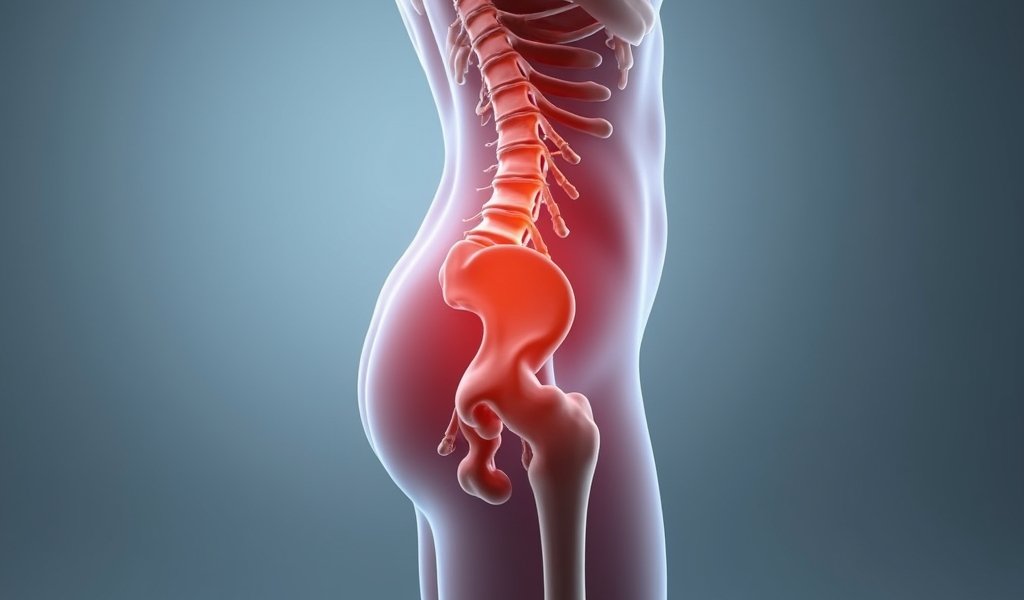
Once the cause of your buttock pain has been identified, treatment can be tailored accordingly. Here’s a breakdown of common approaches:
Physical Therapy
Physical therapy forms the cornerstone of recovery for most causes of post-hip replacement buttock pain. A qualified physical therapist will design a personalized program that may include:
- Targeted stretching for tight muscles
- Progressive strengthening exercises for weak muscles
- Gait training to correct abnormal walking patterns
- Manual therapy techniques to release tight tissues
- Balance and proprioception exercises
Studies show that patients who fully engage with their physical therapy program experience better outcomes and faster pain resolution. Your physical therapist may also incorporate modalities like ultrasound or electrical stimulation for additional pain relief.
Visit a chiropractic wellness center that offers specialized physical therapy for joint replacement patients to ensure you receive appropriate care tailored to your specific needs.
Medication Management
Various medications help manage different aspects of buttock pain:
- Non-steroidal anti-inflammatory drugs (NSAIDs) reduce inflammation and pain
- Acetaminophen provides pain relief without addressing inflammation
- Muscle relaxants may help if muscle spasms contribute to pain
- Nerve pain medications (like gabapentin) target nerve-related symptoms
- Antibiotics are essential if infection is present
Your doctor will recommend the most appropriate medications based on your pain type, medical history, and potential drug interactions. Always take medications exactly as prescribed and report any side effects promptly.
Injections
Therapeutic injections can provide targeted relief for specific causes:
- Corticosteroid injections reduce inflammation in bursitis or tendinitis
- Trigger point injections help release focal areas of muscle tension
- Nerve blocks temporarily interrupt pain signaling for diagnostic or therapeutic purposes
While injections aren’t typically first-line treatments, they can be valuable tools for breaking pain cycles or providing relief while other treatments take effect. According to research published in the Journal of Pain Research, targeted injections can provide significant relief for many patients with post-surgical pain.
Surgical Interventions
When conservative measures fail to resolve persistent buttock pain, surgical options may be considered:
- Revision surgery to address implant positioning or loosening
- Surgical release of tight tissues causing impingement
- Repair of damaged tendons
- Removal and replacement of infected prostheses
The decision to pursue additional surgery is complex and highly individualized. Your surgeon will carefully weigh potential benefits against risks, particularly since revision surgeries typically have higher complication rates than primary procedures.
Recovery and Pain Management Strategies
Beyond formal medical treatments, several strategies can help you manage buttock pain during recovery:
Home Exercise Program
Consistently performing your prescribed exercises between physical therapy sessions accelerates recovery. Your program will likely progress through phases:
- Initial range of motion and isometric exercises
- Progressive resistance training as healing advances
- Functional movements mimicking daily activities
- Balance and proprioception training
Track your exercise compliance in a journal or app – research shows patients who perform their home exercises at least 80% of the time recover faster and experience less pain.
Activity Modification
Temporarily adjusting your activities can reduce pain while tissues heal:
- Avoid prolonged sitting on hard surfaces
- Use cushions designed for hip replacement patients
- Take frequent position breaks during stationary activities
- Temporarily avoid high-impact activities
- Distribute daily activities to prevent overexertion
The goal isn’t to avoid activity entirely but to find the right balance that promotes healing without excessive irritation. Your tolerance will gradually increase over time.
Heat and Cold Therapy
These simple interventions can provide significant relief:
- Ice (15-20 minutes) reduces acute inflammation and pain
- Heat (15-20 minutes) relaxes muscles and increases blood flow
- Contrast therapy (alternating heat and cold) may help stubborn pain
Many patients find ice most helpful after activity that increases pain, while heat works better for morning stiffness or before exercises. Experiment to discover what provides you the most relief.
Sleep Optimization
Quality sleep promotes healing and pain reduction:
- Use pillows strategically for proper alignment (between knees for side-sleeping)
- Consider a mattress topper for additional support
- Establish a relaxing bedtime routine
- Time pain medication appropriately if pain disrupts sleep
Poor sleep worsens pain perception, creating a difficult cycle. Breaking this cycle through improved sleep habits can significantly reduce your overall discomfort.
Complementary Approaches
Consider these additional pain management strategies:
- Gentle massage of non-surgical areas
- Relaxation techniques and mindfulness meditation
- Acupuncture (with provider approval)
- Aquatic therapy in warm water
Studies have demonstrated that multi-modal pain management approaches are more effective than relying on a single strategy. Work with your healthcare team to develop a comprehensive plan tailored to your specific needs.
Prevention Tips and Long-Term Care
While some causes of buttock pain aren’t entirely preventable, these strategies can minimize your risk and optimize long-term outcomes:
Pre-Surgical Preparation
Patients who enter surgery stronger typically experience less post-operative pain:
- Participate in “prehabilitation” exercises prescribed by your physical therapist
- Strengthen core and hip muscles within your pre-surgical limitations
- Optimize nutrition for tissue healing (adequate protein and vitamins)
- Address modifiable risk factors like smoking and blood sugar control
Research shows that patients who participate in pre-surgical strengthening programs experience 20-30% faster functional recovery and less post-operative pain.
Maintain Healthy Weight
Each additional pound places 4-6 pounds of pressure on your hip joint during walking. Maintaining healthy weight reduces stress on your new hip and surrounding tissues, potentially decreasing pain and extending implant longevity.
If weight management is challenging, consider working with a dietitian who specializes in orthopedic patients. Even modest weight reduction of 5-10% can significantly impact joint stress.
Follow Post-Operative Precautions
Your surgeon will provide specific guidelines based on your surgical approach and individual factors:
- Adhere to movement restrictions during the initial healing period
- Use assistive devices as recommended (walkers, canes)
- Progress activity gradually rather than rushing recovery
- Avoid high-risk positions that could stress your hip
Patients who carefully follow post-operative protocols experience fewer complications and less buttock pain during recovery.
Long-Term Joint Protection
After recovery, protect your hip replacement for years to come:
- Maintain strong core and hip muscles through regular exercise
- Choose joint-friendly activities (swimming, cycling, walking)
- Use proper body mechanics for lifting and daily activities
- Attend recommended follow-up appointments
Modern hip replacements can last 15-20+ years with proper care. Your ongoing commitment to joint health plays a significant role in this longevity and your continued comfort.
When to Seek Medical Help
While some discomfort is expected during recovery, certain situations warrant prompt medical attention:
Emergency Situations
Seek immediate emergency care for:
- Sudden, severe pain with inability to bear weight (possible dislocation)
- Chest pain or sudden shortness of breath (possible blood clot to lungs)
- High fever with increasing hip pain (possible infection)
- Significant new bleeding or drainage from the incision
- New onset of severe numbness or inability to move your leg
These situations represent potentially serious complications that require immediate evaluation and treatment.
Non-Emergency Concerns
Contact your surgeon’s office promptly for:
- Pain that steadily worsens instead of improving
- New swelling, redness, or warmth around the surgical site
- Persistent fever (even low-grade)
- Pain that significantly limits your prescribed therapy exercises
- New clicking, grinding, or instability sensations
Early intervention for these issues can prevent more serious complications and keep your recovery on track.
Regular Follow-Up
Even without concerning symptoms, maintain your scheduled follow-up appointments, typically at:
- 2-3 weeks post-surgery
- 6-8 weeks post-surgery
- 3-6 months post-surgery
- 1 year post-surgery
- Then every 1-2 years for monitoring
These appointments allow your surgeon to identify potential issues before they cause significant problems and ensure your implant remains properly positioned and functioning optimally.
Conclusion
Buttock pain after hip replacement is a common experience during the recovery journey. Understanding its many potential causes helps you distinguish between normal healing discomfort and signs of complications requiring medical attention.
Most patients find their buttock pain gradually resolves within 3-6 months as tissues heal, muscles strengthen, and your body adapts to the new joint. The combination of appropriate medical treatment, dedicated physical therapy, and consistent home management strategies optimizes your recovery potential.
Remember that your recovery timeline is unique to you. Avoid comparing your progress to others or rushing through rehabilitation. Instead, focus on gradual improvement, celebrate your milestones, and maintain open communication with your healthcare team.
With patience and proper care, your hip replacement can provide years of improved mobility and quality of life. The temporary discomfort of recovery gives way to the lasting benefits of reduced pain and enhanced function that inspired your surgical journey.
Frequently Asked Questions
How long does buttock pain typically last after hip replacement?
Most patients experience improving buttock pain for 6-12 weeks after surgery, with significant relief by 3 months. Complete resolution may take 6-12 months in some cases, particularly if nerve irritation is involved.
Can sleeping positions affect buttock pain after hip replacement?
Yes, improper sleeping positions can worsen buttock pain by placing stress on healing tissues. Most surgeons recommend sleeping on your back with a pillow between your legs or on the non-operative side with pillows maintaining proper alignment.
Is it normal for buttock pain to be worse than hip pain after replacement surgery?
Many patients are surprised to find buttock pain more prominent than hip pain after surgery, particularly with posterior surgical approaches. This is normal and typically related to gluteal muscle and sciatic nerve irritation during the procedure.
Can physical therapy make buttock pain worse initially?
Some patients experience temporary increases in buttock pain when beginning physical therapy as muscles are challenged and scar tissue is mobilized. This should be short-lived, with overall improvement following as tissues adapt to the exercises.
Could my buttock pain be coming from my back rather than my hip replacement?
Yes, back problems frequently cause referred pain to the buttock area and can be mistaken for hip-related issues. Your healthcare provider can perform specific tests to determine if your spine might be contributing to your symptoms.
