Overview
Whoever said “knee pain is just a flesh wound” clearly never tore their ACL and battled the subsequent balloon-animal-like swelling that follows! This article provides effective strategies for managing ACL tear swelling through immediate care (RICE method), medication, physical therapy, compression garments, proper nutrition, and long-term management techniques, while emphasizing the importance of recognizing warning signs that require medical attention.
Table of Contents
- Understanding ACL Tears and Why Swelling Occurs
- Immediate Care: First 72 Hours After Injury
- The RICE Method: Your First Line of Defense
- Medication Options for Controlling Inflammation
- Physical Therapy Techniques to Reduce Swelling
- Compression Garments: Do They Really Help?
- Nutrition and Hydration for Faster Recovery
- Long-Term Management of ACL Recovery
- When to Worry: Red Flags That Require Medical Attention
- Conclusion
- Frequently Asked Questions
Understanding ACL Tears and Why Swelling Occurs
Dealing with swelling from ACL tear injuries can be one of the most challenging aspects of the recovery process. As an orthopedic specialist, I’ve guided countless patients through this journey, and I understand how frustrating the persistent swelling can be. The anterior cruciate ligament (ACL) is one of the key stabilizers in your knee, and when it tears, your body immediately launches a protective inflammatory response.
This swelling is actually your body’s natural healing mechanism kicking into high gear. When an ACL tear occurs, blood vessels rupture, allowing blood and fluid to fill the joint space. Your immune system then sends specialized cells to the area, bringing more fluid with them to help remove damaged tissue and begin repairs. While necessary for healing, excessive or prolonged swelling can slow your recovery and cause additional discomfort.
Most patients notice significant swelling within hours of the injury, often accompanied by warmth, redness, and that characteristic tight, balloon-like feeling in the knee. This initial inflammatory response typically peaks within 48-72 hours but can persist for weeks without proper management. Understanding why this swelling occurs is the first step toward effectively addressing it.
Immediate Care: First 72 Hours After Injury
The actions you take immediately after an ACL tear can significantly impact your overall recovery timeline and comfort level. During the first 72 hours post-injury, your primary goal should be to limit swelling from ACL tear as much as possible. This critical window sets the stage for your entire healing process.
First, stop any activity immediately when the injury occurs. Continuing to bear weight or “walking it off” can increase damage and subsequent swelling. Next, elevate your leg above heart level whenever possible—this simple position shift uses gravity to help drain excess fluid away from your knee.
Apply ice to the injured area for 15-20 minutes every 2-3 hours during waking hours. Be sure to wrap the ice in a thin towel to protect your skin from direct contact. During this acute phase, avoid heat applications, alcohol, and anti-inflammatory foods that might increase bleeding and swelling. Instead, focus on gentle rest while keeping the joint protected from further stress.
Many patients make the mistake of testing their injured knee too soon. Remember, even if pain subsides somewhat, the internal healing has only just begun. Follow your doctor’s guidance about weight-bearing limitations strictly during this critical period to avoid setbacks that could prolong your recovery.

The RICE Method: Your First Line of Defense
The RICE protocol remains the gold standard for initial management of swelling from ACL tear injuries, and for good reason. This simple yet effective approach helps control inflammation during those crucial first days and can significantly reduce your discomfort.
Here’s how to implement RICE properly:
- Rest: Give your knee the break it needs. Use crutches if recommended by your healthcare provider to avoid putting weight on the injured leg.
- Ice: Cold therapy constricts blood vessels, reducing blood flow and fluid buildup in the injured area. Apply for 15-20 minutes every 2-3 hours, but never directly on skin.
- Compression: An elastic bandage or compression sleeve provides gentle, even pressure that helps prevent excessive fluid accumulation. Ensure it’s snug but not tight enough to impair circulation.
- Elevation: Keep your injured leg raised above heart level whenever possible, especially when icing. This position uses gravity to help drain excess fluid away from the knee.
According to research published in the Journal of Orthopaedic & Sports Physical Therapy, consistent application of the RICE protocol during the first 72 hours can reduce swelling by up to 40% compared to rest alone. The key is consistency—following this approach diligently rather than sporadically will yield the best results.
While RICE provides excellent initial management, remember it’s just the first step in a comprehensive recovery plan. As the acute phase passes, you’ll gradually transition to more active rehabilitation strategies while continuing to monitor and manage any recurring swelling.
Medication Options for Controlling Inflammation
Medications can play an important role in managing swelling from ACL tear injuries, especially during the early stages when inflammation is at its peak. However, it’s essential to use them appropriately and under medical guidance.
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) and naproxen (Aleve) work by blocking enzymes that promote inflammation. These over-the-counter options can be effective for short-term swelling management, usually taken for 7-10 days following injury. Some physicians recommend waiting 48-72 hours after the initial injury before starting NSAIDs, as there’s some evidence suggesting they may interfere with the body’s natural initial healing response.
Acetaminophen (Tylenol) offers pain relief without the anti-inflammatory action, making it a good option if you’re unable to take NSAIDs due to stomach issues, kidney problems, or if you’re in the very early stage of healing. For more severe cases, your doctor might prescribe stronger anti-inflammatory medications or occasionally recommend a corticosteroid injection to reduce significant swelling that isn’t responding to other treatments.
It’s worth noting that while medications can provide relief, they should complement rather than replace other swelling management strategies. Always follow dosing instructions carefully, and discuss any concerns with your healthcare provider, especially if you have underlying health conditions or take other medications that might interact.
Physical Therapy Techniques to Reduce Swelling
Physical therapy isn’t just about rebuilding strength and mobility—it’s also one of your most powerful tools for managing persistent swelling from ACL tear injuries. A skilled physical therapist employs various techniques that can significantly reduce fluid retention while promoting healing.
Gentle range-of-motion exercises help pump excess fluid out of the joint by activating your body’s natural lymphatic drainage system. These controlled movements—often starting with simple ankle pumps, heel slides, and quad sets—stimulate circulation without stressing the healing ligament. Your therapist will gradually progress these exercises as healing allows.
Manual lymphatic drainage, a specialized form of gentle massage, can be remarkably effective for stubborn swelling. This technique uses light, rhythmic strokes to stimulate lymph flow and direct fluid away from the injured knee. Many patients report immediate relief following these sessions.
Electrical stimulation therapy, particularly neuromuscular electrical stimulation (NMES), serves a dual purpose in ACL recovery. While primarily used to prevent muscle atrophy and maintain strength, these gentle electrical impulses also help reduce swelling by improving circulation and lymphatic flow. Your physical therapist might incorporate this modality into your sessions or teach you to use a home unit.
One often overlooked aspect of managing joint inflammation during recovery is maintaining proper movement patterns. Your therapist will ensure you’re not compensating in ways that might increase knee stress and subsequent swelling. This personalized guidance is invaluable for long-term recovery success.
Compression Garments: Do They Really Help?
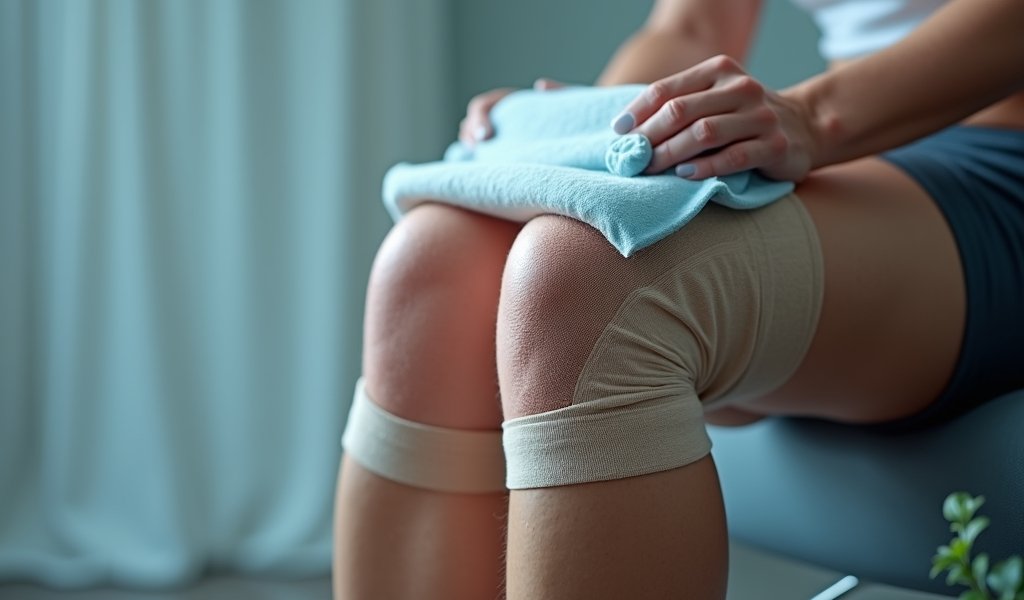
Compression garments have gained popularity as a swelling management tool for ACL injuries, but do they live up to the hype? The evidence suggests they can indeed be valuable when used correctly. Properly fitted compression sleeves, stockings, or wraps provide gentle, consistent pressure that helps prevent excess fluid buildup while supporting the injured joint.
The key benefit of compression for swelling from ACL tear recovery is its ability to improve venous return and lymphatic drainage. By applying graduated pressure (stronger at the ankle, gentler moving up the leg), these garments help push stagnant fluid upward and out of the injured area. This not only reduces visible swelling but can also alleviate the heavy, tight sensation many patients describe.
When choosing compression garments, look for medical-grade products with the appropriate compression level (usually 20-30 mmHg for knee injuries). Avoid garments that feel uncomfortably tight, cause numbness, or create a throbbing sensation—these signs indicate the compression may be too strong. Many rehabilitation specialists recommend wearing compression during daytime hours, especially when you’ll be upright or active, and removing it for sleep.
According to research in sports medicine journals, patients who use compression garments consistently report less swelling and greater comfort during ACL rehabilitation compared to those who don’t. While they’re not a standalone solution, compression garments can be a valuable addition to your recovery toolkit.
Nutrition and Hydration for Faster Recovery
What you eat and drink plays a surprisingly significant role in managing swelling from ACL tear recovery. Your body needs specific nutrients to repair damaged tissue while efficiently processing and eliminating excess fluid.
Protein is the foundation of tissue repair, so ensure you’re getting adequate amounts—generally 1.2-1.6 grams per kilogram of body weight daily during recovery. Focus on quality sources like lean meats, fish, eggs, dairy, and plant-based options like legumes and tofu. Collagen-rich foods such as bone broth can be particularly beneficial for ligament healing.
Anti-inflammatory foods deserve a prominent place in your recovery diet. Include plenty of colorful fruits and vegetables, especially berries, cherries, leafy greens, and cruciferous vegetables like broccoli and cauliflower. Omega-3 fatty acids found in fatty fish, walnuts, and flaxseeds help regulate inflammation, while herbs and spices like turmeric, ginger, and garlic provide additional anti-inflammatory compounds.
Proper hydration is absolutely crucial for managing swelling. When adequately hydrated, your body can more efficiently transport nutrients to healing tissues and remove waste products. Aim for at least 2-3 liters of water daily, more if you’re active or in hot weather. Some patients find that tart cherry juice or pineapple juice (which contains bromelain) helps with inflammation while contributing to hydration needs.
What you avoid matters too. Limit processed foods high in refined carbohydrates, unhealthy fats, and sodium, as these can promote inflammation and fluid retention. Alcohol and excessive caffeine may also interfere with optimal healing and hydration, so moderate or eliminate these during your recovery period.
Long-Term Management of ACL Recovery
As you progress beyond the initial weeks after your ACL tear, managing occasional swelling becomes part of a broader long-term recovery strategy. Even months into rehabilitation, you may notice that your knee swells after certain activities or at the end of a busy day. This is normal and typically responds well to proactive management.
Developing a maintenance routine is essential for long-term success. This might include regular strength training focused on the quadriceps, hamstrings, and core—muscle groups that support proper knee biomechanics and reduce stress on the healing ACL. Balance exercises further enhance joint stability, which can prevent compensatory movements that might trigger swelling.
Activity modification doesn’t mean giving up the things you love, but rather adapting how you approach them. For instance, if running causes swelling, you might incorporate more cross-training with swimming or cycling. Listen to your body’s feedback—swelling is often an indication that you’ve exceeded your current capacity.
Many successful ACL recovery patients adopt a “prehab” mindset, performing maintenance exercises and self-care routines even after formal rehabilitation ends. These might include regular foam rolling, targeted stretching, and prophylactic icing after more demanding activities. This proactive approach helps manage minor swelling before it becomes problematic.
According to long-term follow-up studies, patients who maintain their rehabilitation exercises for at least 9-12 months post-surgery show better outcomes and fewer complications, including less chronic swelling. Remember that full ligament maturation takes approximately two years, so patience with your body’s healing process is essential.
When to Worry: Red Flags That Require Medical Attention
While some degree of swelling from ACL tear injuries is expected throughout recovery, certain symptoms warrant immediate medical attention. Recognizing these red flags can help you distinguish between normal healing responses and potential complications.
Sudden, severe increases in swelling, especially when accompanied by intense pain, could indicate a new injury or disruption to the healing process. If your knee balloons dramatically overnight or after minimal activity, contact your healthcare provider promptly. Similarly, warmth, redness, and tenderness that worsen rather than improve may signal an infection, particularly if you’ve had surgical repair.
Fever developing alongside knee swelling is never normal and requires immediate medical evaluation. This combination often indicates infection, which can have serious consequences if not addressed quickly. Additionally, if you notice unusual drainage from a surgical site, don’t wait to seek care—this could also indicate an infectious process.
Persistent numbness, tingling, or color changes in your foot or lower leg might suggest circulatory issues or nerve compression, potentially related to swelling or treatment methods. These symptoms should never be ignored, as they can lead to more permanent problems if not addressed promptly.
Finally, if swelling consistently interferes with your prescribed rehabilitation exercises despite following all management strategies, consult your healthcare team. They may need to adjust your treatment plan or investigate underlying issues that could be impeding your recovery. Remember, proactive communication with your medical team is always better than waiting until problems escalate.
Conclusion
Managing swelling from ACL tear injuries is a crucial aspect of your recovery journey that directly impacts both your comfort and healing timeline. By implementing the eight essential strategies we’ve discussed—from immediate RICE protocol application to long-term activity modification—you can significantly reduce inflammation and accelerate your return to normal activities.
Remember that consistency is key when combating swelling. The patients who experience the most successful recoveries are those who diligently apply these techniques throughout their rehabilitation process, not just when symptoms become bothersome. Be patient with your body and understand that healing an ACL tear is a marathon, not a sprint.
Your recovery may have challenging moments, but with proper swelling management techniques and the guidance of qualified healthcare professionals, you’ll progress steadily toward full function. Stay committed to your rehabilitation program, listen to your body’s feedback, and celebrate the small victories along the way. Before you know it, that troublesome swelling will become a distant memory as you return to the activities you love.
Frequently Asked Questions
How long does swelling from ACL tear typically last?
Initial significant swelling usually lasts 2-4 weeks after injury or surgery. Mild to moderate swelling may continue intermittently for 3-6 months, especially after activity increases.
Can I exercise with a swollen knee after ACL tear?
Light, approved exercises can continue with mild swelling as long as they don’t increase pain or swelling. Always follow your physical therapist’s guidance and avoid activities that consistently worsen symptoms.
Is it normal for swelling to come and go months after ACL surgery?
Yes, fluctuating swelling is common during the first year of recovery, especially after increased activity. If swelling becomes severe or doesn’t respond to rest and ice, consult your healthcare provider.
Should I wear a compression sleeve at night for ACL swelling?
Most medical professionals recommend removing compression garments at night to allow normal circulation during sleep. Instead, focus on elevation and ensure the sleeve isn’t too tight when worn during the day.
What foods should I avoid to reduce knee swelling after ACL tear?
Limit processed foods high in refined sugars, unhealthy fats, and sodium which can promote inflammation. Alcohol and excessive caffeine may also interfere with healing and increase fluid retention.
