Overview
Ankle-versaries are no fun, but knowing the difference between sprains and fractures is crucial for proper healing! This article provides a complete guide to distinguishing between ankle sprains and fractures, offering diagnostic methods, healing strategies, recovery timelines, prevention tips, and clear guidance on when medical attention is necessary.
Table of Contents
- Understanding Ankle Injuries: Sprains vs Fractures
- Key Differences Between Ankle Sprains and Fractures
- Diagnosis Methods for Ankle Injuries
- 7 Proven Tips to Heal Ankle Injuries Faster
- Recovery Timeline: What to Expect
- When to See a Doctor: Red Flags
- Prevention Strategies for Future Ankle Injuries
- Conclusion
- Frequently Asked Questions
Understanding Ankle Injuries: Sprains vs Fractures
Ankle injuries can happen in an instant – a misstep on uneven ground, a sudden twist during sports, or even something as simple as missing a step. The pain and swelling that follow can leave you wondering: is this an ankle sprain vs fracture? Understanding the difference is crucial for proper treatment and optimal healing.
According to the American Academy of Orthopedic Surgeons, ankle sprains account for approximately 25,000 injuries daily in the United States, making them one of the most common musculoskeletal injuries. Meanwhile, ankle fractures make up about 15% of all ankle injuries, with roughly 184 fractures occurring per 100,000 people annually.
As a healthcare professional specializing in sports medicine, I’ve treated countless ankle injuries over my career. The first thing to understand is that while both injuries affect the same area, they involve different structures and require different approaches to treatment.
A sprain occurs when the ligaments that connect bones are stretched or torn. The ankle has several ligaments that can be damaged, most commonly on the lateral (outside) part of the ankle. On the other hand, a fracture is a break in one or more of the three bones that make up the ankle joint: the tibia, fibula, and talus.
Both injuries can cause significant pain and limit mobility, but proper identification is the first step toward effective recovery. Let’s explore how to tell them apart and the best evidence-based strategies to get you back on your feet faster.
Key Differences Between Ankle Sprains and Fractures
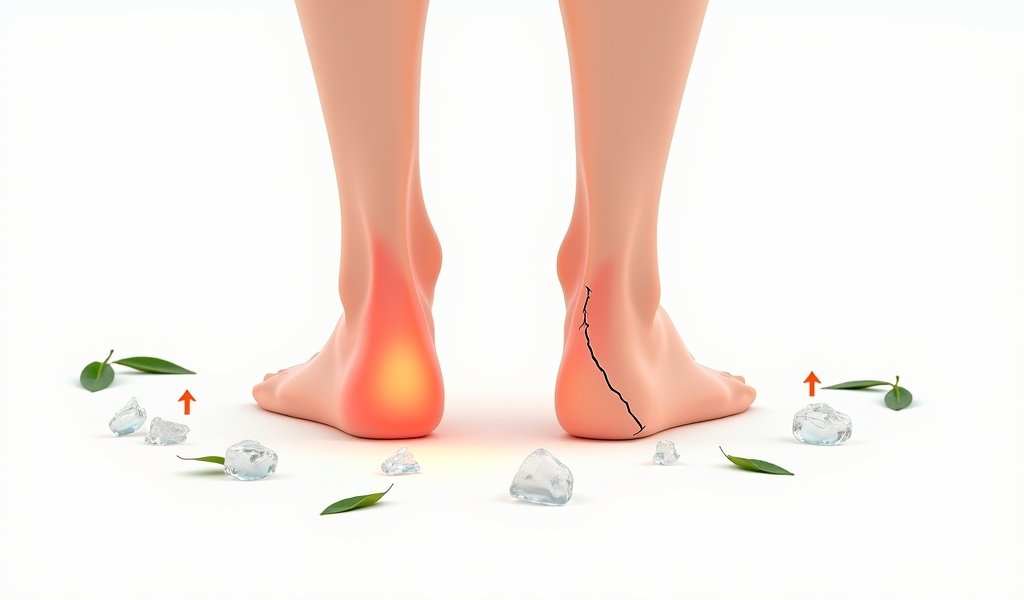
Distinguishing between an ankle sprain and fracture can be challenging, especially in the moments right after injury when pain and swelling dominate the experience. However, several key differences can help identify what you’re dealing with.
With sprains, pain typically localizes over the affected ligament, most commonly on the outside of the ankle. You might still be able to bear some weight, though it will be painful. Swelling tends to develop gradually, and bruising may appear after 24-48 hours.
Fractures, in contrast, often present with more intense, sharp pain that increases significantly with movement or weight-bearing. According to research published in the Journal of Orthopaedic & Sports Physical Therapy, approximately 50% of patients with ankle fractures report hearing a “crack” or “pop” at the moment of injury. Swelling typically develops rapidly, and bruising appears sooner and can be more extensive.
Another important distinction lies in mobility. With a sprain, you might still maintain some range of motion, albeit painful. A fracture typically severely restricts movement and attempting to move the ankle causes sharp, intense pain. Research from the Journal of Clinical Medicine found that inability to bear weight immediately after injury and for four steps during emergency department assessment was 95% sensitive for identifying clinically significant ankle fractures.
It’s worth noting that severe (grade III) sprains can sometimes be as debilitating and painful as fractures, which is why proper medical assessment is essential for serious ankle injuries.
Diagnosis Methods for Ankle Injuries
Accurate diagnosis is crucial for proper treatment of ankle injuries. As someone who has worked closely with chiropractic and wellness specialists, I’ve seen firsthand how the right diagnostic approach makes all the difference in recovery outcomes.
Your healthcare provider will typically start with a physical examination. They’ll check for specific areas of tenderness, swelling, bruising, and assess your range of motion. The Ottawa Ankle Rules, a validated clinical decision tool, helps determine whether X-rays are necessary. These rules have been shown to reduce unnecessary radiographs by up to 30-40% while maintaining nearly 100% sensitivity for identifying fractures.
For suspected sprains, your doctor will perform specific tests to check ligament stability. The anterior drawer test and the talar tilt test evaluate the integrity of the lateral ligaments. These hands-on assessments can reveal a lot about the nature and severity of your injury.
When imaging is needed, X-rays are typically the first choice for suspected fractures. They can clearly show bone breaks but won’t reveal soft tissue damage like ligament tears. A study published in the American Journal of Roentgenology found that approximately 13-17% of ankle fractures are missed on initial X-rays, which is why additional views or follow-up imaging might be necessary.
For more complex cases, advanced imaging might be recommended:
- MRI scans provide detailed images of both bones and soft tissues, making them excellent for diagnosing ligament tears and subtle fractures.
- CT scans offer detailed 3D views of bones, helpful for complex fractures or surgical planning.
- Ultrasound can be useful for evaluating soft tissue injuries and is increasingly used for point-of-care assessment.
Remember, self-diagnosis can lead to improper treatment. If you’re dealing with significant pain, inability to bear weight, or visible deformity, seeking professional medical evaluation is essential for proper diagnosis and care.
7 Proven Tips to Heal Ankle Injuries Faster
Whether you’re dealing with a sprain or fracture, certain evidence-based strategies can significantly accelerate your healing process. As someone who provides comprehensive wellness services to patients with various injuries, I’ve compiled these seven proven tips to optimize your recovery:
1. Follow the R.I.C.E. Protocol Initially
The R.I.C.E. method (Rest, Ice, Compression, Elevation) remains a cornerstone of initial injury management. For the first 48-72 hours, rest the injured ankle, apply ice for 15-20 minutes every 2-3 hours, use a compression bandage, and keep your foot elevated above heart level when possible. Research published in the Journal of Athletic Training shows this approach can reduce swelling by up to 47% compared to no treatment.
2. Progress to Early Controlled Movement
Contrary to older beliefs about complete immobilization, current evidence supports early controlled movement for most ankle injuries. A systematic review in the British Journal of Sports Medicine found that early mobilization led to faster return to work and sport, less pain, and less swelling compared to immobilization. For sprains, gentle ankle circles and alphabet exercises (tracing the alphabet with your toes) can begin as early as 48-72 hours after injury, as pain allows.
3. Optimize Your Nutrition for Healing
Your body needs specific nutrients to repair damaged tissues. Ensure adequate protein intake (1.2-1.6g per kg of body weight daily) to support tissue repair. Vitamin C is essential for collagen formation, while zinc, vitamin D, and calcium support bone healing. A study in the Journal of Bone and Mineral Research found that vitamin D deficiency can delay fracture healing by up to 3-4 weeks.
4. Engage in Appropriate Physical Therapy
Working with a qualified physical therapist can accelerate recovery by 2-3 weeks compared to self-directed rehabilitation. Physical therapy typically includes progressive strengthening, proprioception training, and functional exercises tailored to your specific injury and goals. Research shows that supervised rehabilitation reduces re-injury rates by up to 35%.
5. Consider Evidence-Based Supplements
Certain supplements may support tissue healing. A 2017 meta-analysis found that collagen supplementation (10-15g daily) improved joint pain and function in athletes with ankle injuries. Curcumin (1000-1500mg daily with piperine for better absorption) has been shown to reduce inflammation and pain. Always consult your healthcare provider before starting any supplement regimen.
6. Use Appropriate Supportive Devices
For sprains, a semi-rigid ankle brace or athletic tape can provide support while allowing beneficial movement. For fractures, following your orthopedist’s recommendations for casting, booting, or post-surgical protocols is essential. A study in the American Journal of Sports Medicine found that using an appropriate brace during the rehabilitation phase reduced re-injury risk by 56% compared to no bracing.
7. Prioritize Quality Sleep
Sleep is when your body does much of its repair work. Aim for 7-9 hours of quality sleep per night. Research published in the International Journal of Sports Medicine demonstrated that athletes who slept less than 6 hours per night experienced 30% slower healing rates than those sleeping 8+ hours. Consider elevating your ankle during sleep to further reduce nighttime swelling.
Implementing these evidence-based strategies consistently can significantly accelerate your recovery from both ankle sprains and fractures. As always, these recommendations should complement, not replace, your healthcare provider’s specific instructions for your unique injury.
Recovery Timeline: What to Expect
Knowing what to expect during recovery can help you set realistic expectations and stay motivated through the healing process. As a healthcare professional focused on physical wellness, I’ve guided countless patients through ankle injury recovery, and understanding the typical timeline is incredibly helpful.
For ankle sprains, recovery typically follows this pattern:
- Grade I (Mild) Sprains: 1-3 weeks for full healing
- Grade II (Moderate) Sprains: 3-6 weeks for substantial recovery
- Grade III (Severe) Sprains: 8-12 weeks or longer for complete healing
According to a comprehensive review in the Journal of Orthopedic Research, approximately 80% of individuals with Grade I-II ankle sprains return to normal activities within 6 weeks. However, studies show that up to 40% of people report some lingering symptoms like occasional pain or feelings of instability for up to 6-12 months after a moderate to severe sprain.
For ankle fractures, the timeline varies significantly based on the type and severity:
- Stable, non-displaced fractures: 6-8 weeks for bone healing
- Displaced fractures requiring surgery: 12-16 weeks for initial healing
- Complex fractures: Up to 20 weeks or longer before full weight-bearing
Complete functional recovery, including return to sports and high-impact activities, typically takes 4-6 months for most fractures. Research from the Journal of Bone and Joint Surgery indicates that about 85% of patients with surgically treated ankle fractures achieve good to excellent functional outcomes by 12 months post-injury.
It’s important to note that these timelines represent averages. Individual factors like age, overall health, compliance with treatment protocols, and commitment to rehabilitation exercises can significantly impact recovery speed. Older adults typically heal more slowly than younger individuals, and those with conditions like diabetes or peripheral vascular disease may experience extended healing times.
Throughout your recovery, you’ll progress through several phases:
- Acute Phase (0-72 hours): Focus on minimizing swelling and protecting the injury
- Early Recovery (Days 3-14): Gradual introduction of gentle range of motion exercises
- Middle Recovery (Weeks 2-6): Progressive strengthening and proprioception training
- Late Recovery (6+ weeks): Return to function and sport-specific training
Remember that healing is rarely linear. You might experience plateaus or even temporary setbacks along the way. This is normal and doesn’t mean your overall recovery isn’t progressing. Patience and consistency with your rehabilitation program are key to optimal outcomes.

When to See a Doctor: Red Flags
While many ankle injuries can be managed with home care, certain signs and symptoms warrant immediate medical attention. As a healthcare professional, I’ve seen the complications that can arise from delayed treatment of serious ankle injuries.
Seek medical care promptly if you experience any of these red flags:
- Inability to bear any weight on the affected foot
- Visible deformity or misalignment of the ankle
- A popping or cracking sound at the time of injury
- Severe swelling or bruising that develops rapidly
- Numbness, tingling, or loss of sensation in the foot
- Skin that is cold, pale, or turning bluish
- Pain that is unbearable or increases significantly despite rest and basic care
- Open wound or bone protruding through the skin (seek emergency care immediately)
According to research published by the American Academy of Family Physicians, delayed treatment of certain ankle fractures can increase the risk of complications by up to 60%, including malunion (improper healing), chronic pain, and post-traumatic arthritis.
For children and adolescents, it’s particularly important to seek medical evaluation for ankle injuries. Their growing bones include growth plates that, if damaged and not properly treated, can lead to long-term growth abnormalities. Studies show that up to 18% of pediatric ankle injuries involve the growth plate.
Even if your injury initially seems minor, monitor for evolving symptoms. If swelling, pain, or bruising worsens rather than gradually improving over the first 72 hours, or if you develop fever, redness, or warmth around the injury site (potential signs of infection), consult a healthcare provider promptly.
Remember that early, accurate diagnosis and appropriate treatment significantly improve long-term outcomes. A study in the Journal of Foot and Ankle Research found that patients who received appropriate care within the first week of injury had 40% better functional outcomes at six months compared to those who delayed seeking treatment.
Prevention Strategies for Future Ankle Injuries
After experiencing an ankle sprain or fracture, you’ll naturally want to avoid going through it again. The good news is that implementing specific prevention strategies can significantly reduce your risk of recurrence. Research published in the British Journal of Sports Medicine shows that appropriate prevention programs can reduce ankle injury rates by 30-50%.
Here are evidence-based strategies to protect your ankles:
Strengthen Your Ankle Complex
Strong muscles around the ankle provide crucial support and stability. Focus on exercises that strengthen all four directions of ankle movement: dorsiflexion (pulling toes up), plantarflexion (pointing toes), inversion (turning sole inward), and eversion (turning sole outward). A systematic review found that consistent strength training reduced ankle injury risk by approximately 35% in athletes with previous ankle injuries.
Improve Balance and Proprioception
Proprioception—your body’s awareness of position and movement—is often impaired after ankle injuries. Single-leg balance exercises, wobble board training, and other balance challenges can restore and enhance this crucial sense. Research shows that proprioceptive training can reduce ankle sprain recurrence by up to 86% in previously injured individuals.
Choose Appropriate Footwear
Shoes that provide adequate support for your specific foot type and activity level are essential. A study in the American Journal of Sports Medicine found that basketball players wearing shoes with proper ankle support experienced 47% fewer ankle injuries than those wearing low-top shoes without support. If you have high arches or overpronate, consider custom or over-the-counter orthotics for additional support.
Use Preventive Bracing or Taping When Appropriate
For high-risk activities, especially if you have a history of ankle injuries, consider prophylactic bracing or taping. A meta-analysis of 31 studies found that external ankle supports reduced the risk of ankle sprains by approximately 70% in individuals with previous sprains. Semi-rigid braces appear to offer the best balance of protection and performance.
Warm Up Properly
Never skip your warm-up, especially before activities involving running, jumping, or quick direction changes. Dynamic warm-ups that gradually increase blood flow and prepare the tissues for activity have been shown to reduce overall injury rates by 30-50%. Include ankle-specific movements like circles, alphabets, and gentle plyometrics.
Train Smart
Gradually increase training intensity, duration, and frequency to allow your tissues to adapt appropriately. The “10% rule”—not increasing your training load by more than 10% per week—is a good guideline to follow. Research shows that rapid increases in training volume correlate strongly with increased injury rates.
By implementing these prevention strategies consistently, you’ll significantly reduce your risk of future ankle injuries while optimizing your performance and enjoyment of physical activities. Prevention truly is the best medicine when it comes to ankle health.
Conclusion
Navigating the journey from injury to recovery with an ankle sprain vs fracture can be challenging, but with the right approach, you can minimize downtime and return to your normal activities with confidence. The key differences between these injuries lie in their mechanism, presentation, and treatment requirements – understanding these distinctions is crucial for proper care.
Remember that while the seven healing tips outlined in this article are backed by strong evidence, individual healing journeys vary. Some people recover quickly, while others may need more time and patience. Trust the process and follow your healthcare provider’s guidance.
Prevention remains your best strategy once you’ve recovered. By strengthening your ankles, improving proprioception, wearing appropriate footwear, and training intelligently, you can significantly reduce your risk of future injuries.
Most importantly, listen to your body throughout recovery. Pushing too hard too soon can lead to setbacks, while appropriate progressive challenges help build strength and confidence. The goal isn’t just to heal your current injury but to emerge stronger and more resilient than before.
With patience, consistency, and the evidence-based strategies outlined in this article, you’ll be well-equipped to recover fully from your ankle injury and return to the activities you love.
Frequently Asked Questions
How can I tell if my ankle is broken or just sprained?
Fractures typically involve more intense pain, inability to bear weight, and often a “crack” sound at injury. Sprains usually allow some weight-bearing with pain primarily over the ligament area, though severe sprains can mimic fractures.
Do I need an X-ray for every ankle injury?
Not every ankle injury requires an X-ray. Healthcare providers often use the Ottawa Ankle Rules to determine if imaging is necessary based on specific pain locations and ability to bear weight.
How long should I use crutches after an ankle sprain or fracture?
For moderate sprains, crutches are typically needed for 1-3 days until walking with minimal pain is possible. Fractures usually require 6-8 weeks of limited or non-weight bearing, depending on the fracture type and treatment approach.
Can I exercise with an ankle sprain?
Yes, but modify your routine to avoid activities that cause pain or put stress on the ankle. Swimming, stationary biking with minimal resistance, and upper body workouts are generally safe options during recovery.
Will my ankle ever be the same after a serious sprain or fracture?
With proper rehabilitation, most people regain full or nearly full function after ankle injuries. However, some may experience subtle changes in proprioception or occasional mild symptoms, especially after severe injuries.