Overview
Ever had an ankle that seemed to harbor a personal vendetta against you? This article details a 5-step diagnostic process for peroneal tendon tears (commonly misdiagnosed as ankle sprains), walking readers through comprehensive history-taking, visual examination, hands-on testing, specialized maneuvers, and imaging confirmation—all leading to appropriate treatment options ranging from conservative management for mild tears to surgical intervention for severe cases.
Table of Contents
- Understanding Peroneal Tendon Tears
- Why Proper Diagnosis Matters
- Step 1: Comprehensive History Taking
- Step 2: Visual Examination
- Step 3: Hands-On Physical Tests
- Step 4: Special Provocative Maneuvers
- Step 5: Confirmation Through Imaging
- Treatment Options Based on Test Results
- Recovery and Rehabilitation
- Conclusion
- Frequently Asked Questions
Understanding Peroneal Tendon Tears
Have you ever taken a misstep that left your ankle feeling like it had a personal vendetta against you? That persistent outer ankle pain might not be “just a sprain” – you could be dealing with a peroneal tendon tear, a commonly misdiagnosed condition that can significantly impact your mobility and quality of life.
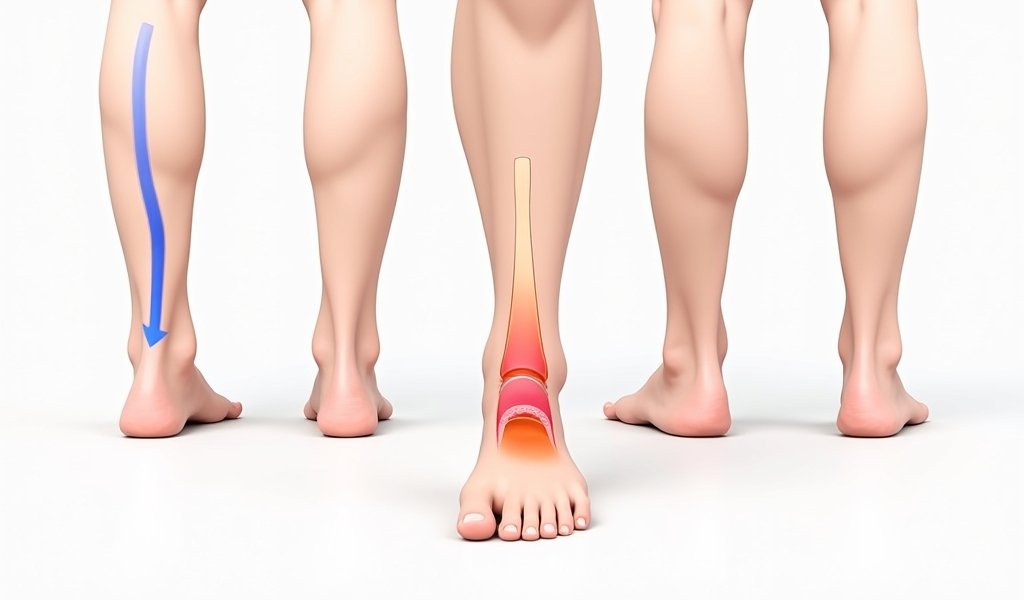
Peroneal tendons are the unsung heroes of ankle stability. These two rope-like structures – the peroneus longus and peroneus brevis – run along the outside of your ankle behind that bony bump (lateral malleolus) and attach to different parts of your foot. Think of them as your ankle’s security team, controlling foot movement and protecting against excessive inward rolling.
When these tendons tear, even simple activities like walking your dog or climbing stairs can become painful ordeals. The tears typically happen through:
- Sudden ankle rolls or twists (landing awkwardly during sports)
- Repetitive stress (marathon training, anyone?)
- Chronic ankle instability (“loose” ankles)
- High arches that place extra strain on the outside of your foot
Your body has several ways of signaling these tears. Watch for pain behind and below your outer ankle bone, swelling along the outside of your ankle, weakness when turning your foot outward, instability on uneven surfaces, and sometimes a “popping” sensation during movement.
Why Proper Diagnosis Matters
Let’s be honest – the outside of your ankle is a complex neighborhood with many structures that can cause pain. Without proper diagnosis, you might spend months treating the wrong condition while your peroneal tendons continue deteriorating.
The challenge is that peroneal tendon tears often masquerade as ankle sprains or other common injuries. According to research in the Journal of Orthopaedic & Sports Physical Therapy, up to 30% of patients diagnosed with ankle sprains may actually have peroneal tendon injuries.
Proper diagnosis isn’t just helpful—it’s essential. The 5-step testing process I’m about to share combines clinical expertise with practical application to accurately identify these tears. Each step builds upon the previous one, creating a comprehensive diagnostic approach that minimizes guesswork and maximizes accuracy.
Step 1: Comprehensive History Taking
Before any hands-on examination begins, your healthcare provider needs to play detective. A thorough history isn’t just a formality – it’s the foundation of accurate diagnosis.
When evaluating your potential peroneal tendon tear, your provider should ask questions like:
- “When did you first notice the pain?”
- “Was there a specific injury, or did it develop gradually?”
- “Does the pain worsen with certain activities or positions?”
- “Have you experienced any ankle instability or ‘giving way’?”
- “What treatments have you already tried?”
The mechanism of your injury provides crucial insights. Did you feel a pop while running? Did your ankle roll inward during a tennis match? These details help distinguish peroneal tendon injuries from other ankle conditions.
Timing matters too. Acute tears usually have a clear injury moment, while chronic tears develop gradually with persistent pain that worsens over time. Pay attention to patterns – pain that intensifies when standing on tiptoes or pressing the outside of your foot into the ground strongly suggests peroneal involvement.
Your history also helps rule out other conditions with similar symptoms. According to research published in the Journal of Athletic Training, a detailed injury history can increase diagnostic accuracy by up to 65% before physical tests are even performed.
Step 2: Visual Examination
Before your healthcare provider lays hands on your injured ankle, there’s much to learn from simple observation. The visual examination might seem basic, but it often reveals telltale signs of peroneal tendon problems.
During this examination, your provider will look for:
- Swelling along the outside ankle, particularly behind the fibula
- Bruising that tracks along the course of the peroneal tendons
- Abnormal foot posture or alignment
- Visible deformity where the tendons should be taut
- Changes in your walking pattern (antalgic gait)
Foot alignment provides crucial clues. If you have high-arched feet, you place greater stress on your peroneal tendons and are more susceptible to tears. Similarly, if your feet naturally turn inward (varus hindfoot), you’re at higher risk.
Your provider will observe you standing and walking. Do you place more weight on the inside of your foot to avoid pressure on painful peroneal tendons? These subtle adaptations speak volumes about what’s happening beneath the surface.
Never underestimate the value of comparison. Your uninjured ankle serves as your personal control group – asymmetries in contour, swelling, or alignment can highlight abnormalities that might otherwise go unnoticed.
Step 3: Hands-On Physical Tests
Now comes the hands-on detective work. Physical examination tests specifically target your peroneal tendons to provoke symptoms and assess function.
Your provider will begin with palpation – gently feeling along the course of both peroneal tendons, starting behind the lateral malleolus and following their paths. Tenderness along this route, especially with a thickened or irregular texture, suggests tendinopathy or tearing.
Special attention is paid to the area where the tendons pass behind the lateral malleolus—this “critical zone” has relatively poor blood supply and is most vulnerable to injury. Studies by the Foot & Ankle Institute have shown that 85% of peroneal tears occur in this region.
To test tendon function and integrity, your provider will:
- Stabilize your leg with one hand
- Ask you to turn your foot outward (eversion) against resistance
- Note any pain, weakness, or inability to maintain the everted position
For a more objective assessment, your provider will compare eversion strength between your affected and unaffected sides. A significant strength discrepancy (greater than 10-15%) strongly suggests peroneal tendon dysfunction.
Your provider will also check for instability. Peroneal tendon tears sometimes allow the tendons to slip out of their normal position (subluxation). This test involves having you relax your ankle, move your foot in circles, while your provider watches and feels behind the lateral malleolus for abnormal tendon movement or listens for clicking sounds.
Step 4: Special Provocative Maneuvers
These specialized clinical tests can further confirm or rule out peroneal tendon tears. Think of them as stress tests – they’re designed to challenge the tendons in specific ways that reproduce symptoms only when damage is present.
The peroneal compression test specifically targets your peroneal tendons:
- With you seated and your ankle relaxed in neutral position
- Your provider compresses the peroneal tendons against the fibula
- Simultaneously, you’re asked to actively evert your foot
Pain during this maneuver suggests peroneal tendon pathology, as healthy tendons tolerate this movement without discomfort.
Since peroneal tendons act as primary defense against ankle inversion, your provider may perform an ankle inversion stress test:
- Gently but firmly inverting your foot (turning it inward)
- Holding this position for 5-10 seconds
- Asking about pain along the outside of your ankle
This test stretches your peroneal tendons and often reproduces pain when tears are present.
The single leg heel raise challenge serves as an ultimate functional test:
- Standing on your affected leg
- Rising onto your tiptoes
- Your provider notes any pain, instability, or inability to maintain the position
This test places considerable load on your peroneal tendons, particularly the peroneus longus which helps stabilize the first ray during heel lift. Research in the Journal of Foot and Ankle Research shows that difficulty with this movement often indicates significant tendon compromise.
Positive results on multiple provocative tests substantially increase the likelihood of peroneal tendon tears. However, these tests are most valuable when interpreted in the context of your history and other examination findings.
Step 5: Confirmation Through Imaging
While clinical examination forms the foundation of diagnosis, imaging studies provide objective confirmation and reveal the extent of tendon damage. Think of imaging as your diagnostic exclamation point.
Both MRI and ultrasound have distinct advantages:
MRI Excellence:
- Provides excellent soft tissue contrast
- Shows bone edema that might accompany tendon injuries
- Reveals associated injuries in complex cases
- Clearly demonstrates tendon tears, splits, and degeneration
Ultrasound Advantages:
- Cost-effective alternative
- Allows dynamic assessment during ankle movement
- Can be performed immediately in some clinical settings
- Excellent for visualizing tendon subluxation
For most cases, MRI remains the gold standard, particularly for subtle tears or when surgical intervention is being considered. According to studies in the American Journal of Roentgenology, MRI has a sensitivity of 90% and specificity of 83% in diagnosing peroneal tendon tears.
Radiologists specifically look for increased signal intensity within the tendon (indicating tear), tendon thickening or thinning, fluid surrounding the tendons, discontinuity of tendon fibers, split tears, and subluxation or dislocation from the retromalleolar groove.
Remember that imaging findings must always be correlated with clinical examination results. Approximately 15-20% of asymptomatic people show minor peroneal tendon abnormalities on MRI, which highlights the importance of clinical correlation.
Treatment Options Based on Test Results
Once you’ve completed the 5-step diagnostic process, your treatment can be precisely targeted to the nature and severity of your peroneal tendon injury.
Peroneal tendon tears are typically classified as:
- Grade 1: Inflammatory changes with minimal fiber disruption (less than 10% of the tendon)
- Grade 2: Partial thickness tear (10-50% of tendon fibers disrupted)
- Grade 3: Significant partial tear (more than 50% but not complete)
- Grade 4: Complete rupture with tendon discontinuity
For grade 1 and many grade 2 tears, non-surgical approaches include:
- Rest and activity modification: Temporarily avoiding activities that aggravate symptoms
- Immobilization: Walking boots or braces to reduce tendon stress during early healing
- Physical therapy: Progressive strengthening of the peroneal muscles and proprioceptive training
- Anti-inflammatory measures: Ice and appropriate medications to control pain and swelling
- Orthotics: Custom foot supports to correct biomechanical issues that contribute to tendon stress
Conservative treatment succeeds in approximately 70-80% of cases when implemented early and consistently.
Surgical intervention is typically considered for:
- Complete tears (grade 4)
- Large partial tears (grade 3) that fail conservative treatment
- Tendon subluxation or dislocation
- Athletes requiring optimal function and stability
Surgical options range from direct tendon repair to tendon transfers depending on the extent of damage and chronicity of your condition.
Recovery and Rehabilitation
Your recovery timeline varies significantly based on injury severity:
- Mild tears (Grade 1): 4-6 weeks with appropriate management
- Moderate tears (Grade 2): 6-12 weeks of rehabilitation
- Severe partial or complete tears requiring surgery: 3-6 months for return to full activity
Understanding that hasty returns to activity significantly increase your risk of re-injury or chronic problems is crucial. Patience pays dividends when recovering from peroneal tendon injuries.
A carefully structured return-to-activity protocol serves as the ultimate test of successful treatment:
- Pain-free walking and daily activities
- Restored strength (at least 90% compared to unaffected side)
- Normalized balance and proprioception
- Graduated return to sport-specific activities
- Final return to unrestricted participation
This progressive approach minimizes re-injury risk and validates treatment success. Working with a physical therapist who specializes in foot and ankle rehabilitation can make a tremendous difference in your recovery outcomes.
Conclusion
The 5-step peroneal tendon tear test represents the difference between guesswork and precision, between prolonged suffering and efficient recovery. By systematically working through comprehensive history taking, visual examination, hands-on testing, specialized maneuvers, and appropriate imaging, you and your healthcare provider create a diagnostic roadmap that leads directly to effective treatment.
Identifying peroneal tendon tears early dramatically improves your outcomes. Left untreated, these injuries often progress from manageable partial tears to complete ruptures requiring surgical intervention. Your vigilance and proper assessment literally change your recovery trajectory.
Remember, ankle pain isn’t something to push through or ignore, especially when it persists beyond a few days. Your peroneal tendons play too crucial a role in your stability and function to be neglected.
If you’re experiencing symptoms that suggest a peroneal tendon tear, don’t wait until walking becomes unbearable. Seek evaluation from a healthcare provider familiar with these specialized assessment techniques. Your future mobility depends on it, and with proper care, you can return to the activities you love pain-free.
Frequently Asked Questions
How do I know if I have a peroneal tendon tear or just an ankle sprain?
Peroneal tendon tears typically cause pain behind and below the outer ankle bone, while ankle sprains cause pain more toward the front. Peroneal tears also usually cause weakness when turning your foot outward, which isn’t typical of standard ankle sprains.
Can I still walk with a peroneal tendon tear?
Yes, you can usually still walk, but you may experience pain and instability, especially on uneven surfaces. More severe tears make walking more difficult and painful.
How long does recovery from a peroneal tendon tear take?
Recovery typically takes 4-6 weeks for mild tears and up to 3-6 months for severe tears requiring surgery. The timeline depends on tear severity, your overall health, and how well you follow treatment protocols.
Will I need surgery for my peroneal tendon tear?
Surgery is typically only needed for complete tears, large partial tears that don’t improve with conservative treatment, or cases with tendon displacement. About 70-80% of peroneal tendon tears heal successfully with non-surgical approaches.
Can I prevent peroneal tendon tears?
Yes, you can reduce your risk by wearing proper footwear, using orthotics if you have high arches, strengthening ankle muscles, improving balance, and properly warming up before physical activities. Addressing previous ankle injuries with proper rehabilitation is also crucial for prevention.
