Overview
Turns out your ear and jaw are such close neighbors that when one catches an infection, the other feels compelled to join the pity party with radiating pain! This article explains how ear infections cause jaw discomfort through anatomical connections, details symptoms to watch for, and provides five practical relief strategies including pain management, hot/cold therapy, gentle exercises, dietary adjustments, and treating the underlying infection.
Table of Contents
- Understanding the Connection Between Ear Infections and Jaw Pain
- How Ear Infections Cause Jaw Pain: The Anatomical Explanation
- Symptoms to Watch For: When Jaw Pain Might Be from an Ear Infection
- Relief Tip #1: Appropriate Pain Management Strategies
- Relief Tip #2: Hot and Cold Therapy Applications
- Relief Tip #3: Gentle Jaw Exercises and Stretches
- Relief Tip #4: Dietary Modifications to Reduce Pain
- Relief Tip #5: Treating the Underlying Ear Infection
- When to See a Doctor About Ear-Related Jaw Pain
- Prevention Strategies for Ear Infections and Associated Jaw Pain
- Conclusion
- Frequently Asked Questions
Understanding the Connection Between Ear Infections and Jaw Pain
If you’ve ever experienced an ear infection accompanied by jaw pain, you’re not alone. This uncomfortable duo affects millions of Americans each year, creating a particularly unpleasant experience that can disrupt daily activities. The question “can ear infection cause jaw pain?” has a straightforward answer: absolutely yes.
Ear infections, while primarily affecting the ear structure, commonly radiate pain to surrounding areas—with the jaw being a frequent casualty. This isn’t coincidental but rather a direct result of the close anatomical relationship between these structures. Understanding this connection can help you identify the true source of your discomfort and seek appropriate treatment.
The proximity between your ear and jaw creates an environment where inflammation from an ear infection can easily spread to the jaw region. When infection develops in the ear, the resulting inflammation, pressure, and fluid buildup don’t always respect anatomical boundaries. Instead, they can extend their reach to neighboring structures, including the temporomandibular joint (TMJ) that connects your jawbone to your skull.
Recognizing this relationship is crucial for proper treatment. Too often, people mistake ear infection-related jaw pain for dental issues, leading to unnecessary dental visits and treatments that won’t address the root cause. By understanding that your jaw discomfort might stem from an ear problem, you can seek appropriate health and wellness care right from the start.
How Ear Infections Cause Jaw Pain: The Anatomical Explanation
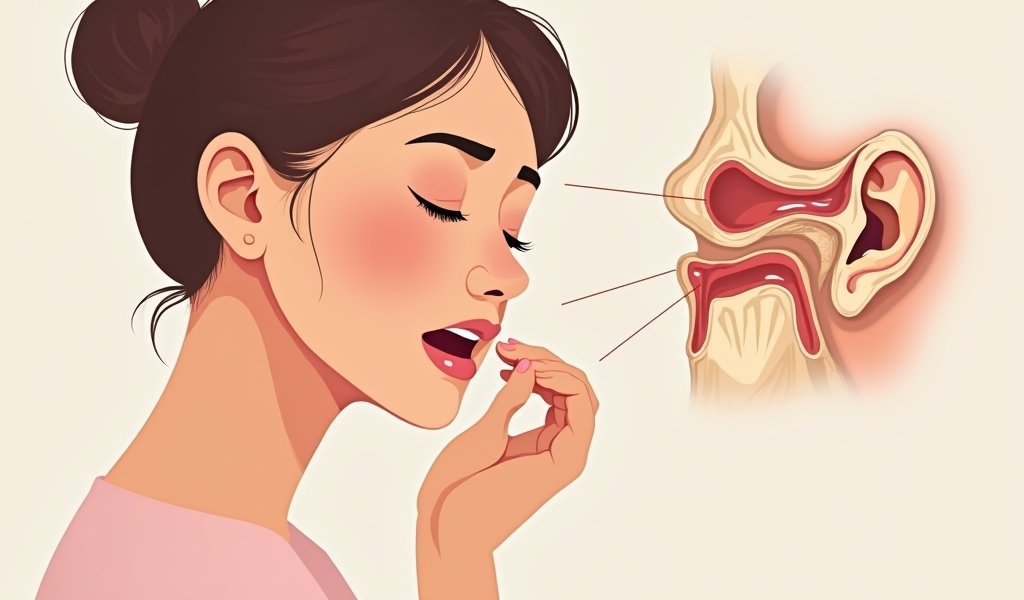
To understand how an ear infection triggers jaw pain, we need to explore the intimate anatomical relationship between these structures. Your ear isn’t just an isolated organ—it’s part of a complex network that includes nerves, muscles, joints, and other tissues that interconnect with surrounding areas.
The temporomandibular joint (TMJ) sits immediately adjacent to your ear canal. In fact, if you place your finger just in front of your ear and open your mouth, you can feel this joint moving. This proximity means that inflammation from an ear infection doesn’t have far to travel to affect your jaw joint.
Middle ear infections (otitis media) are particularly notorious for causing jaw pain. According to research published in the Journal of Clinical Medicine, when infection causes the middle ear to become inflamed, several mechanisms can trigger jaw discomfort:
- Direct pressure from fluid buildup in the ear pushing against structures near the jaw
- Inflammation spreading through connected tissue pathways
- Referred pain through shared nerve pathways between the ear and jaw
- Muscle tension from holding the jaw in uncomfortable positions to minimize ear pain
External ear infections (otitis externa) can similarly cause jaw pain, particularly when significant swelling occurs in the ear canal. This swelling can press against the TMJ or irritate the muscles that control jaw movement.
Children are especially vulnerable to this ear-jaw connection. Their Eustachian tubes—passages that connect the middle ear to the back of the throat—are shorter, more horizontal, and functionally different from adults. This anatomical difference makes children more susceptible to ear infections and, consequently, the jaw pain that often accompanies them.
Symptoms to Watch For: When Jaw Pain Might Be from an Ear Infection
Distinguishing jaw pain caused by an ear infection from other potential causes can be challenging. However, certain patterns and accompanying symptoms can help you identify when your jaw discomfort might be ear-related.
When an ear infection is the culprit behind your jaw pain, you’ll likely notice these telltale signs:
- Pain that seems to radiate from the ear area toward the jaw
- Increased jaw discomfort when pulling on the earlobe or applying pressure near the ear
- Pain that worsens with jaw movements like chewing, talking, or yawning
- Accompanying ear symptoms such as fullness, pressure, itching, or discharge
- Reduced hearing clarity or muffled sounds in the affected ear
- Occasional fever, especially with middle ear infections
Unlike TMJ disorders, ear infection-related jaw pain typically doesn’t involve clicking, grinding, or locking sensations when moving the jaw. The pain pattern also differs from dental problems, as it doesn’t usually worsen with temperature changes or sweet foods.
Children might not articulate their symptoms clearly, so watch for behavioral cues like tugging at the ears, increased irritability, trouble sleeping, or reluctance to eat due to chewing discomfort. These signs, especially when accompanied by fever or ear drainage, warrant prompt medical evaluation at a wellness clinic near you.
Remember that viral upper respiratory infections often precede ear infections, so recent cold symptoms followed by ear discomfort and jaw pain suggest an infectious process rather than a primary TMJ problem.
Relief Tip #1: Appropriate Pain Management Strategies
When ear infection-related jaw pain strikes, appropriate pain management becomes a priority. Over-the-counter analgesics can provide significant relief while the infection resolves, either naturally or with medical intervention.
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) or naproxen sodium (Aleve) work particularly well for this type of pain because they address both pain and inflammation. Take them with food to minimize stomach irritation, and follow package instructions for proper dosing.
Acetaminophen (Tylenol) can also help manage pain, though it lacks the anti-inflammatory properties of NSAIDs. For some individuals, especially those with stomach sensitivities or who are taking certain medications, acetaminophen might be the safer choice. The American Academy of Family Physicians notes that alternating between acetaminophen and ibuprofen can sometimes provide enhanced pain relief while minimizing side effects.
For more severe pain, your healthcare provider might prescribe stronger medications or ear drops with anesthetic properties. These prescription options are typically reserved for cases where over-the-counter remedies prove insufficient.
Importantly, pain management should be viewed as a temporary measure while addressing the underlying ear infection. Simply masking the pain without treating the infection can lead to prolonged discomfort and potential complications.
Relief Tip #2: Hot and Cold Therapy Applications
Temperature therapy offers a simple yet effective approach to managing ear infection-related jaw pain. Both heat and cold applications have their place in your relief toolkit, with each providing distinct benefits.
Heat therapy works by increasing blood flow to the affected area, relaxing tense muscles, and providing a soothing sensation that can temporarily override pain signals. For ear-related jaw pain, try:
- Applying a warm (not hot) compress to the jaw area for 15-20 minutes
- Using a microwavable heat pack wrapped in a thin towel
- Taking a warm shower, allowing the heat to reach your face and jaw
Cold therapy, on the other hand, reduces inflammation by constricting blood vessels and numbing nerve endings. This approach works well during acute pain flares:
- Wrap an ice pack or frozen vegetables in a thin cloth and apply to the jaw for 10-15 minutes
- Use a cold gel mask designed for facial application
- Alternate between cold and warm applications, with 20-30 minutes between treatments
Many people find that alternating between heat and cold provides optimal relief. You might start with cold therapy to reduce initial inflammation, then switch to heat to improve circulation and relaxation. This combination approach has shown effectiveness in clinical research on musculoskeletal pain.
Remember to always place a barrier between your skin and the temperature source to prevent tissue damage, and limit applications to 20 minutes maximum with adequate rest periods between treatments.
Relief Tip #3: Gentle Jaw Exercises and Stretches
When an ear infection causes jaw pain, gentle exercises and stretches can help maintain mobility and reduce muscle tension. These movements should never force the jaw beyond comfortable limits or cause increased pain.
Start with these simple, effective exercises:
- Controlled opening: Place your fingers on your jaw joint (just in front of your ears) and slowly open your mouth to a comfortable width, hold for 5 seconds, then gently close. Repeat 5-10 times.
- Lateral movements: With your teeth slightly apart, move your lower jaw slowly from side to side within a comfortable range. Perform 10 repetitions.
- Resistance exercise: Place your thumb under your chin and create gentle resistance as you slowly open your mouth halfway. Hold for 5 seconds, then close. Repeat 5 times.
- Relaxation technique: Rest your tongue lightly on the roof of your mouth behind your front teeth, then let your teeth come apart slightly to relax the jaw muscles.
These exercises work best when performed several times daily, but always with gentleness as the guiding principle. Stop immediately if any exercise increases pain or discomfort.
For additional benefit, combine these exercises with gentle self-massage of the jaw muscles. Using your fingertips, apply moderate pressure in small circular motions along the jawline and in front of the ears. This can help release tension that develops as a protective response to ear-related pain.
Health and wellness experts recommend performing these exercises in a warm environment, ideally after applying gentle heat to the area, as warmth increases tissue flexibility. Morning and evening routines often work well for most people.
Relief Tip #4: Dietary Modifications to Reduce Pain
What you eat can significantly impact jaw comfort when dealing with ear infection-related pain. Modifying your diet temporarily can reduce strain on tender jaw muscles and joints while supporting your body’s healing process.
Focus on incorporating these jaw-friendly foods:
- Soft, easy-to-chew options: Yogurt, smoothies, pureed soups, scrambled eggs, and well-cooked pasta
- Protein-rich soft foods: Cottage cheese, hummus, refried beans, and soft-cooked fish
- Nutrient-dense options: Avocados, well-cooked vegetables, applesauce, and nutritional supplement drinks
Equally important is avoiding foods that require excessive chewing or jaw movement:
- Tough meats like steak or jerky
- Crunchy items like raw carrots, apples, or hard bread crusts
- Chewy foods like bagels, caramels, or taffy
- Very hot or cold foods that might trigger pain responses
Maintaining proper hydration is crucial during an ear infection, as dehydration can potentially worsen inflammation and slow healing. Opt for room-temperature water rather than ice-cold beverages, which might trigger pain in sensitive teeth or jaw areas.
Nutritionists at Nutrition.gov recommend eating smaller, more frequent meals rather than three large ones when dealing with jaw pain. This approach reduces fatigue in the jaw muscles and minimizes discomfort.
Remember that these dietary modifications are temporary measures to support comfort during recovery—not long-term restrictions. Once your ear infection and associated jaw pain resolve, you can gradually reintroduce your normal diet.
Relief Tip #5: Treating the Underlying Ear Infection
The most effective way to relieve ear infection-related jaw pain is to address the root cause—the infection itself. Treatment approaches vary depending on whether the infection is bacterial, viral, or fungal in nature.
For bacterial ear infections, which are common in middle ear cases (otitis media), antibiotics are often prescribed. If your doctor recommends this treatment, it’s crucial to:
- Take the full course of antibiotics exactly as prescribed, even if symptoms improve before finishing
- Keep track of when doses are due to maintain consistent antibiotic levels
- Report any adverse reactions to your healthcare provider promptly
Many ear infections, particularly viral ones, resolve without antibiotics. In these cases, supportive care becomes paramount:
- Use over-the-counter ear drops designed to relieve pain (with your doctor’s approval)
- Apply warm compresses to the affected ear several times daily
- Take appropriate pain relievers as discussed in Relief Tip #1
- Get plenty of rest to support your immune system’s fight against infection
For outer ear infections (otitis externa or “swimmer’s ear”), your doctor might prescribe antibiotic ear drops, sometimes combined with steroid components to reduce inflammation. Keeping the ear dry during treatment is essential for recovery.
Complementary approaches like staying well-hydrated, using a humidifier to prevent mucous membranes from drying out, and avoiding irritants like cigarette smoke can support faster healing. These measures help create an optimal environment for recovery while antibiotics or your immune system tackle the infection.
When to See a Doctor About Ear-Related Jaw Pain
While mild ear infections and associated jaw pain sometimes resolve without medical intervention, certain scenarios warrant prompt professional attention. Recognizing these situations can prevent complications and ensure appropriate treatment.
Seek medical care if you experience:
- Severe pain that significantly impacts your ability to function or sleep
- Pain persisting beyond 2-3 days, especially if worsening rather than improving
- Fever above 102°F (38.9°C) in adults or any fever in infants
- Discharge from the ear, particularly if bloody or resembling pus
- Sudden hearing loss or significant changes in hearing ability
- Dizziness, coordination problems, or facial weakness
- Swelling behind the ear or abnormal protrusion of the ear
For children, the threshold for seeking medical care should be lower. Children under six months with suspected ear infections should always be evaluated by a healthcare provider, as should any child with severe symptoms or signs of ear infection following a respiratory illness.
During your medical visit, be prepared to describe:
- When symptoms began and how they’ve progressed
- Whether pain is constant or intermittent
- What makes the pain better or worse
- Any recent illnesses, particularly respiratory infections
- Previous ear problems or treatments
Remember that telemedicine options are increasingly available for initial assessment of ear infection symptoms. These virtual visits can help determine whether in-person evaluation is necessary and might provide interim relief recommendations.
Prevention Strategies for Ear Infections and Associated Jaw Pain
While not all ear infections are preventable, several strategies can significantly reduce your risk and help avoid the accompanying jaw discomfort. Incorporating these practices into your routine can support long-term ear health.
Practice good ear hygiene by:
- Keeping ears dry after swimming or bathing
- Using ear protection in contaminated water
- Avoiding insertion of objects into the ear canal, including cotton swabs
- Using alcohol-based ear drops after swimming if recommended by your doctor
Support your immune system with:
- Adequate sleep and stress management
- Regular physical activity appropriate for your fitness level
- A balanced diet rich in fruits, vegetables, and immune-supporting nutrients
- Staying current with recommended vaccinations
Manage environmental factors by:
- Avoiding cigarette smoke and other respiratory irritants
- Promptly treating allergies and upper respiratory infections
- Using a humidifier in dry environments to maintain healthy mucous membranes
- Practicing good hand hygiene to reduce exposure to infectious agents
For those prone to recurrent ear infections, additional preventive measures might include surgical interventions like ear tubes in children with frequent middle ear infections or specialized earplugs for swimmers.
Research from the Centers for Disease Control and Prevention indicates that breastfeeding infants for at least six months can reduce ear infection frequency. Similarly, keeping children away from secondhand smoke significantly lowers their infection risk.
Conclusion
The connection between ear infections and jaw pain highlights the intricate relationships within our body’s structures. When infection takes hold in the ear, the inflammatory response doesn’t respect neat anatomical boundaries, often extending to create uncomfortable jaw sensations that can disrupt daily activities.
Understanding that ear infections can cause jaw pain is the first step toward appropriate management. By recognizing the signs that distinguish ear-related jaw discomfort from other causes, you can seek timely and appropriate care rather than pursuing treatments that miss the underlying issue.
The five relief tips we’ve explored—pain management, temperature therapy, gentle exercises, dietary adjustments, and treating the underlying infection—provide a comprehensive approach to managing this uncomfortable condition. These strategies work best when implemented together as part of a holistic recovery plan.
Remember that while self-care measures can provide significant relief, certain situations warrant professional medical attention. Severe or persistent symptoms, particularly when accompanied by fever, hearing changes, or unusual discharge, should prompt a healthcare consultation.
By incorporating preventive strategies into your routine and responding appropriately when infections do occur, you can minimize both the frequency and impact of ear infections and their associated jaw discomfort. This proactive approach to ear health contributes to your overall wellbeing and quality of life.
Frequently Asked Questions
Can both children and adults experience jaw pain from ear infections?
Yes, both children and adults can experience jaw pain from ear infections. Children may be more susceptible due to their developing ear anatomy and more frequent ear infections.
How long does jaw pain typically last after an ear infection begins?
Jaw pain typically subsides as the ear infection resolves, usually within 5-7 days with proper treatment. Persistent jaw pain beyond two weeks warrants further medical evaluation.
Can ear infection-related jaw pain be confused with TMJ disorders?
Yes, ear infection-related jaw pain can be mistaken for temporomandibular joint (TMJ) disorders. The key difference is that ear infection pain usually accompanies other ear symptoms like pressure, fullness, or hearing changes.
Is jaw pain more common with certain types of ear infections?
Jaw pain occurs most frequently with middle ear infections (otitis media) due to the proximity to the jaw joint. However, outer ear infections (otitis externa) can also cause jaw discomfort, especially when significant swelling is present.
Can antibiotics help relieve jaw pain caused by ear infections?
Antibiotics don’t directly relieve pain but treat the underlying bacterial infection causing inflammation. As the infection resolves, related jaw pain typically diminishes within 2-3 days of starting antibiotic treatment.
